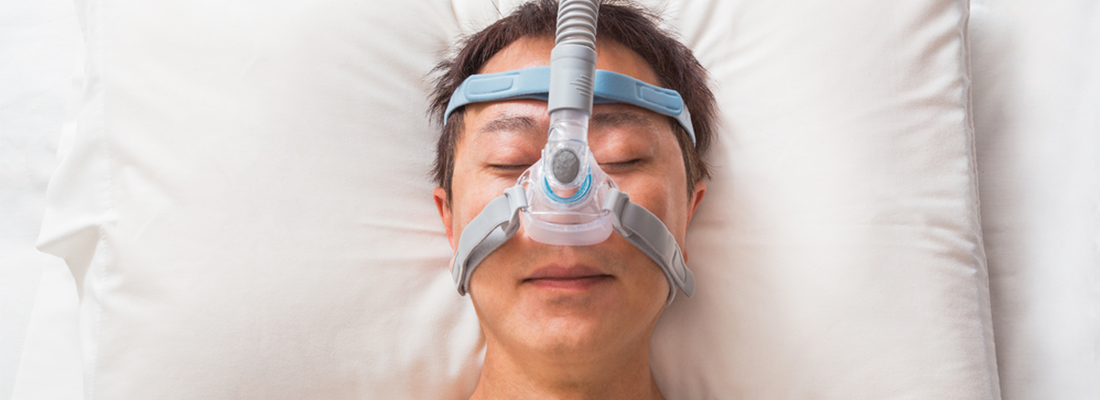
Wearing CPAP is difficult. Here are some problems that new users encounter.
CPAP stands for Continuous Positive Airway Pressure. It is the gold standard for the treatment of Obstructive Sleep Apnea (OSA). The apparatus consists of an air pump (that provides either a fixed or variable pressure), a warm humidifier, and tubing that connects to a facial mask. This isn’t a ventilator that breathes for you. The positive air pressure maintains the “open-ness (the medical term is patency) of collapsible airways while you sleep. Over the past few years CPAP machines have vastly improved over older models. They are quiet, efficient, and, if used, very effective at preventing airway blockage for a person with OSA. Additionally, the machine collects data while you use it, including the number of hours it is worn and the effectiveness of the pressure setting. That information can be transmitted to “the cloud” for you, your physician, the company that supplies the machine, and potentially your insurance company.
First developed in the early 80s, and improved in the 90s with better and more comfortable masks, CPAP is the most prescribed, and most effective, treatment for OSA. There is even a CPAP unit used for people who just snore without apnea. As of 2014 it was estimated that more than 1 million Americans have used CPAP.
The problem is that everyone who is prescribed CPAP isn’t able to succeed, or they choose to stop using the machine due to discomfort or inconvenience. Wearing that mask every night for the rest of your life can be disheartening and discouraging. Even if you did well during a CPAP study in a sleep lab (formally called a pressure titration study), wearing one in your own bed, long term, is a difficult leap for many to take. Up to 50% of people for whom CPAP has been prescribed don’t wear it.
Here are some common problems experienced by some CPAP users:
CPAP is difficult to get accustomed to. Sure, it is. Everyone has a nightly ritual they go through to get ready for bed – brushing your teeth, putting on your Superman PJs, adjusting your pillows, checking the alarm, and turning out the lights to finally end the day. Now add a face mask and head gear that tethers you to an air pressure machine. It is at best disruptive to the comforting and relaxing process you have counted on your whole life. For some people, it just seems “too much” to get used to.
The mask is uncomfortable and leaves marks on the face. Even people who have been wearing a CPAP apparatus for years wake up with strap and mask marks on their faces. Look around the next morning you are in church or synagogue and you may notice the faithful users of their machines. Through the course of a morning these marks will fade. But you can still see them in the mirror every morning when you brush your teeth. To help prevent the “mark of CPAP”, the mask and headgear must be fitted carefully. Your medical device provider should have the expertise to measure you and find a comfortable choice. That said, it is common for new CPAP wearers to go through several masks before they find the right one. And even when it fits well, the mask is still on your face at night. So, comfort is key, but getting used to it is difficult.
The mask “comes off” when I sleep. Not uncommonly, a CPAP mask ends up on the floor by morning time, especially in the initial phase of use. Sometimes going to sleep wearing it is not the issue. Subconsciously, or not, you take it off in the middle of the night, often without remembering. Of course no CPAP mask on the face = no CPAP = no treatment.
CPAP takes maintenance. Keeping your mask and tubing clean is an ongoing task. Warm moist air, saliva, and occasionally snot, may accumulate in your device. Yuck. Regular cleaning is a tedious chore, but necessary. The Sleep Foundation recommends taking the mask and tubing into the shower with you weekly to wash them with a mild soap. Hang it up over the showerhead to dry and by nighttime you are back in business. This may not be the shower companion you prefer, but clean devices are nicer for your nose and airway. There are commercially available daily cleaning devices available. They are expensive but for some people a lot more convenient than cleaning it by hand.
Dry noses and mouths inhibit CPAP use. The introduction of efficient heated, built in humidifiers has gone a long way to alleviate this problem. But some wearers still have issues. Not using the humidifier is tolerated by a minority of CPAP users. Most people do better with it on. This adds another layer of maintenance to your day, though. Distilled water is necessary to prevent the build-up of minerals and deposits in the water reservoir. And that container has to be cleaned regularly, too. Mouth-breathing with a nasal mask can dry you out even if the inhaled air is humidified. Full-face masks are often the answer.
Difficulties breathing comfortably with the mask in place are common. Some people are claustrophobic. Having a mask strapped across your face and around your head creates a sense of suffocation. But most people who have difficulty breathing with CPAP have either have trouble getting used to the air pressure or have an anatomical nasal obstruction. People often adjust to the pressure with time and persistence. Nasal congestion can be a deal breaker though. If a full-face mask is not a comfortable option, and medical management of allergies and nasal inflammation is not enough, nasal procedures to reshape and widen restricted nasal passages should be considered. If you are struggling with your nose and your CPAP machine, talk to your sleep doctor before you give up. Help is available.
IMPORTANT SAFETY AND HEALTH WARNING: If you decide not to treat your Obstructive Sleep Apnea for any of the above reasons, or a hundred others you could concoct, please know that you are putting your health at risk. Untreated OSA is associated with significant cardiovascular disease, weight gain, productivity loss, interpersonal difficulties, and driving and occupational safety issues. Wearing CPAP is not great, for sure. But it is better than the consequences of not wearing a life-saving device.