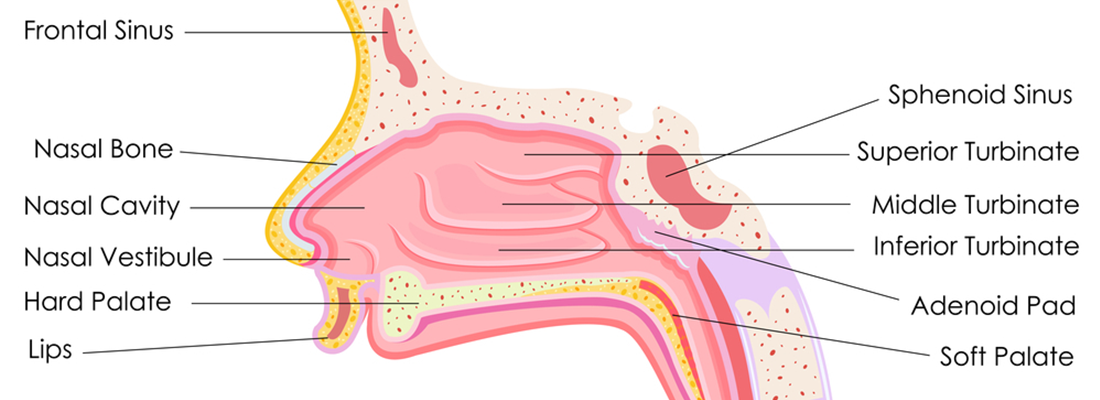
Brief review of surgical procedures to open your nose by correcting obstructive nasal turbinates.
Nasal turbinates, where and what are they?
The turbinates are located on the inside walls of the nose on either side of the septum. They are made of a thin bony shelf surrounded by a vascular soft tissue which is in turn covered by mucosa, just like the rest of the inside of the nose. The blood vessels function to warm the air you inhale. These vessels swell and contract, enlarging or shrinking the turbinates, depending on the amount of blood flowing through them. Mucous glands in the lining moisturize the air in the nose. When the nose is irritated by infection, allergy, or even uneven airflow (due to a deviated nasal septum) the turbinates may enlarge enough to restrict airflow. Increased mucous production is another reaction to inflammation.
How can the turbinates be reduced?
There are a number of procedures that decrease the size of the lower (or inferior) turbinates to decrease nasal congestion. After healing, the smaller turbinates still need to have enough tissue left behind to warm and humidify the air as they are intended to do.
Turbinectomy
A generic term that describes the surgical removal of a portion of the inferior turbinates.
Submucosal Resection
As the name implies, tissue under the mucosa (or nasal lining) is removed. This may include soft tissues and/or the turbinate bones. This is often accomplished using an instrument called a microdebrider. It sucks up and cuts out vascular tissue, decreasing the volume of the turbinate.
Turbinoplasty
This procedure pushes the turbinate to the side. It is often referred to as “outfracture” as the turbinate bones are crushed up against the side of the nose, moving them out of the airway.
These procedures are performed in an operating room and require either sedation (with local numbing medicine injected into the turbinate) or general anesthesia. They are invasive and painful otherwise.
Turbinate Shrinking Procedures: Radiofrequency, Coblation, and Laser Turbinate Ablation
These techniques use heat generated from electrocautery, coblation, or radiofrequency energy to affect the inferior turbinates. A thin instrument is brought in contact with the turbinate mucosa. The injury results in scarring and shrinking of the soft tissue to open the airway.
Post-Operative Care
Pain, fatigue, nasal congestion, and drainage are common after turbinate reduction surgery. Pain is usually mild but may require medication. Congestion due to swelling is short lived, usually improving about a week after the procedure. Slight bleeding or bloody mucous is expected for a few days as well. If there is significant bleeding (very uncommon) during the surgery, packing may be placed and removed several days later.
Keeping the nose moist with antibiotic ointment and/or nasal salt water helps decrease complications and speed healing. Your surgeon will instruct you on to care for yourself after the procedure.